What Causes Adolescent Idiopathic Scoliosis?
First, there are many myths about causation (aetiology).
- It is not a postural problem.
- You do not get scoliosis from a soft mattress.
- The carrying of heavy school bags neither causes a curve nor makes an existing one worse.
- You do not get scoliosis from watching too much television and eating too much junk food.
- Scoliosis is not contagious – you cannot catch it from someone who has a curvature.
A positive family history is a definite risk factor for AIS. Instead of being called idiopathic it would be more correct to say the vast majority of AIS patients have familial (genetic) scoliosis. But, traditions die hard in medicine. There is also sound scientific evidence that undefined ‘environmental’ factors play a role in causation. Hence, it is generally agreed by those who work in this field that the inheritance of AIS is what is termed multifactorial. The yet-to-be identified gene(s) have a very strong tendency to be passed down on the female side. However, there are no hard and fast rules for the pattern of inheritance and a girl or a boy who develops AIS may be the first one to do so in several generations of a family. Much research needs to be done to solve the problem that can be solved and will be solved in time.
If an adolescent is found to have AIS then it is a wise precaution and good medicine that his/her siblings be examined for the condition, but not before the 11th year. The most likely affected first degree relative is a maternal female cousin.
The Outward Signs of Scoliosis
These depend in greater part on where the curve is located in the spine. The curve patterns are named according to the location of the most rotated vertebra(e) which is at the apex of the curve. There are three common single patterns – thoracic, thoracolumbar and lumbar. The second of these has its apex at the junction between the thoracic and lumbar regions. Curves may point in either direction but the right thoracic and left lumbar curves are the most common patterns. A double curve pattern is also common with right thoracic and left lumbar components. The neck (cervical) region is not affected by AIS.
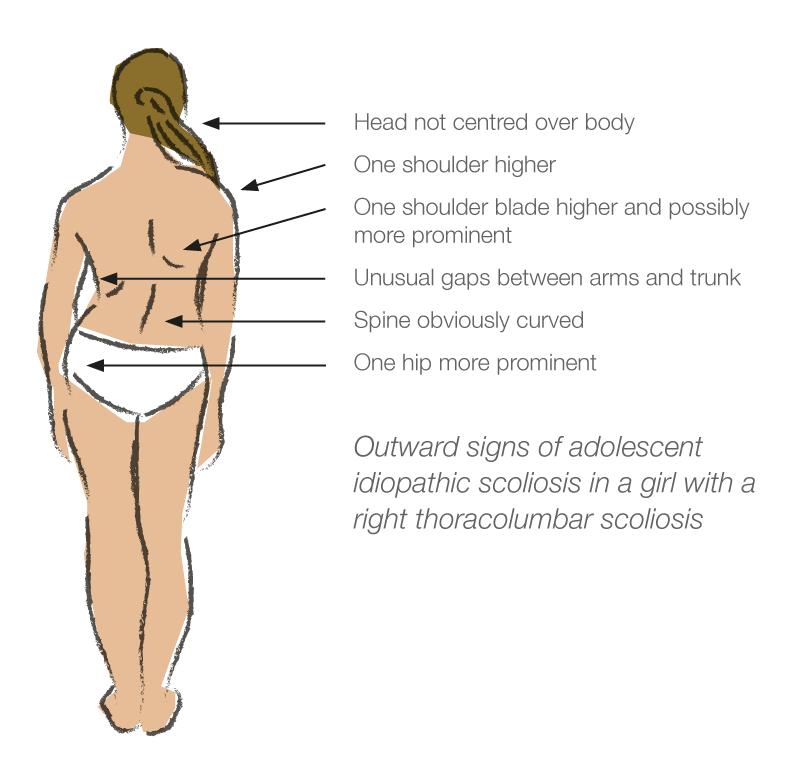
Figure 1 shows the outward signs of AIS in an adolescent girl with a right thoracolumbar scoliosis. These signs, which are less obvious if a girl is overweight, tend to be more marked the higher in the spine is the location of the apex.
Screening For Scoliosis
Where properly conducted school screening programs are carried out these should be supported and participation encouraged. School screening is best performed in girls in Years 5 and 7 (10 and 12 years of age on average). The Spine Society of Australia recommends that if screening is to be restricted on budgetary grounds, it should be limited to girls in Year 7. No case has ever been made for the routine screening of boys.
A two-tier screening process is recommended, the first being by school nurses trained in the Forward Bend Test (FBT – see below). Confirmation of a structural scoliosis by a doctor should take place before a family is notified. Over-diagnosis, a pitfall in screening programs, is best avoided by this two-tier approach. The notification rate should be less than three percent.
The abandonment of school screening programs led to the introduction of the National Scoliosis Detection Program . This entails the distribution of a Scoliosis Detection Fact Sheet to girls in Years 5 and 7 via the school systems. The thrust of this approach is to place responsibility for curve detection on the adolescent population and for management of minor curves on the family doctor. Over-referral to specialists is to be avoided. Most curves do not require active treatment.
The Forward Bend Test
This is the key to the detection of scoliosis and it demonstrates the fixed rotatory component of a curve. In the thoracic region the ribs follow the rotating spine and move posteriorly and upwards, giving a prominence on the side of the apex – a right thoracic curve will have a right thoracic prominence in the FBT. In the lumbar region there are no ribs so with a lumbar curve the muscles on the side of the apex become more prominent. This is called the bolster sign because of the appearance of the prominence being similar to that of a long pillow (bolster). The prominence with thoracolumbar curves is a mixture of the above two described findings Figure 2 demonstrates a correctly performed FBT in the girl shown in Figure 1.

X-Ray Examination
This is required once a clinical diagnosis of all forms of scoliosis is made. Education programs for family doctors and radiologists have been developed to ensure that exposure to x-rays is kept to a minimum. The standard film required for the initial assessment is well within established safety limits.
X-rays are an essential investigation in the assessment of spinal deformities. However, they should only be done when absolutely necessary. In some cases, that could mean up to 2 – 3 times a year, such as in young children whose curves can get bigger when they grow in height quickly.
In general, the following guidelines are reasonable:
1. When a child or teenager is first seen for scoliosis, a standing (erect) X-ray is taken “PA and lateral”. This gives a good view of the spine from the back and the side. In many cases, no more lateral (side) views are needed.
2. On subsequent visits, X-rays are not always needed. X-rays could be done as infrequently as once a year or two in someone whose curve seems stable. They might be needed every six months if treatment such as a brace is being used. If surgery is being planned, special “bending” X-rays are often done.
X-rays should not be done without good reason. There is no scientific reason to have one regularly as part of chiropractic treatment.
3. Spine X-rays should be taken “PA” – that is, with the person’s back to the radiation source (the tube) with the film cassette in front. The reason for this is that a lot of the X-rays “bounce” or scatter off the outer layers of body without passing straight through. The most sensitive tissues to radiation in the field of a spine X-ray are not the ovaries or testes, but breast and thyroid. An X-ray taken PA reduces the radiation dose to those tissues by around 60%, compared to an AP (front to back) film. You should ask that your child has X-rays taken in this manner.
4. Ovaries tend to sit low in the pelvis and are usually out of the field of the X-ray beam. Most spine X-rays only need to see the upper part of the pelvis, above the ovaries. Therefore, shielding is usually not necessary.
5. For most girls and boys with an adolescent idiopathic scoliosis only a few X-rays over number of years are ever needed. That is because most people with scoliosis need no treatment for it. Only 1% of those with a curve will need bracing or surgical treatment. The X-ray dose is low due to better technology, up to 40 times less than prior to 1965.The risk of a cancer or other damage forming due to a series of spinal X-rays over a few years is negligible. However, exposure should be “as low as reasonably achievable”.
Recent published research from Australia has shown no increased cancer risk in children having scoliosis surgery since the 1970s (Do Children with Spinal Deformity who have Metal Implants and Frequent Exposure to X-Rays Increase Their Risk of Cancer? P Cundy, K Venugopal, K D’Onise, G Antoniou, F Brooks, B Freeman, SPINE, 2020 Sep 1;45(17):1200-1207).
6. X-rays, like photographs, can be taken in different ways. The exposure/dose can be reduced, but the quality of the picture may be not as good. Some X-ray practices are very good at lowering the dose for children’s X-rays but still getting a good image. If your city has an EOS scanner and your child is likely to need a number of X-rays due to a progressive scoliosis, you may prefer to go to that centre. Ask your doctor.
Some notes on X-rays:
We are exposed to X-rays (ionising radiation) every day of our lives. In Australia, the average yearly exposure is 2 – 3 milliSieverts (mSv). One-third comes from cosmic radiation, two-thirds from sources on earth, such as some foods, mineral water, rocks such as granite and so on. In some parts of the world, the background levels are much higher (Sweden 6msV, France 5mSv, Kerala, India 50mSv). Cancer rates in these countries are no higher than in places with lower exposures. Air travel exposes us to more radiation, as it increases with altitude. A return flight from Sydney to Perth gives more radiation than a chest X-ray. Living at sea level reduces your exposure compared to high altitude such as Denver, Colorado where background levels are around 3 times higher.
Medical radiation sources (X-rays and CT scans) give varying radiation ‘doses’, depending on the type of scan being done. A chest X-ray uses little radiation (0.03mSv) as the chest is mainly air. A spine X-ray (depending on views taken) gives a dose between 1.5 and 2.5mSv. That dose represents about 6 to 9 months background radiation. EOS scanners, present at some major centres, use far less radiation than standard machines.
CT scanners use high energy X-rays and in some circumstances, can give doses equivalent to several years background radiation. For this reason CT scans are usually only used for special needs such as special diagnostic investigation or pre-operative planning.
Management
First and foremost patients with AIS and their parents must understand that the diagnosis of AIS is a clinical and radiological one. The diagnosis is one of exclusion, that is the exclusion of those conditions such as neuromuscular disorder etc which can produce a curve. There are no biochemical or other markers (blood tests) specific for AIS. Further, there are no markers which will allow a spinal surgeon to predict accurately whether or not a given curve will progress. However, there are sound data on the probability (the risk) or progression as detailed in Table 1.
Risk of Progression of AIS (Females)
| Degree of Curve (Cobb Angle) | Age 10 – 12 | Age 13 – 15 | Age over 16 |
|---|---|---|---|
| < 20 deg | 25% | 10% | 0% |
| 20 – 30 deg | 60% | 40% | 10% |
| 30 – 60 deg | 90% | 70% | 30% |
| > 60 deg | 100% | 90% | 70% |
It is readily deduced from this table that curves are most likely to progress and require active treatment (bracing or surgery) the larger the curve is at presentation and the age at which medical advice is first sought. This is because curves progress most rapidly during the growth spurt – 10-13 years in girls and about 18 months later in boys. These are average figures and averages only appear on paper. Early breast development in girls is a reliable sign of the onset of the spurt. The commencement of periods (menarche) is not reliable in this regard and the average age for this event is 10-15 years, by which time the spurt is over. However, it is dangerous to apply rigid rules to biological events. Every girl and boy is different from all others.
The management of scoliosis centres on regular physical examination through the growth phase with x-rays as required. This is important because curve progression may take place without the patient being aware of any change. Fourth monthly visits are usual in the spurt phase and less frequently thereafter until growth has ceased and the patient is skeletally mature. Here again there are no hard and fast rules.
AIS patients soon become conversant with the ‘angle’ of their curves. This is called the Cobb angle and is measured on the x-ray. The only treatments which are effective in the management of AIS are bracing and surgery. The lay press abounds with claims for success with naturopathy, chiropractic manipulations, exercise programs (physiotherapy), electrical stimulation and so on. None of these supposed treatments can withstand critical analysis. The criterion for success of a given treatment is to produce accurate measurements of the Cobb angle before and after a treatment program and this the above-cited ‘therapies’ cannot do.
Minor curves <25 degrees do not require any treatment and observation only is indicated throughout the growth phase. No restrictions are placed on the young person’s activities. Although scoliosis by definition (a curve of 10° or more) is present in one out of ten adolescent girls, only two to three per thousand come into the active treatment range. The surgery rate is approximately one per thousand.
Brace Treatment
Brace treatment aims to control a curve and contain it at an acceptable angle through the growth phase. It does not ‘cure’ scoliosis. External forces applied to the growing skeleton are very effective in modulating the shape of some structures. For example, orthodontic treatment. Here the braces are firmly attached to the teeth and moreover the young patient attends the orthodontist’s surgery on a regular basis to have the braces tightened. A scoliosis brace does not have this decided mechanical advantage but in suitable candidates for a bracing program who are compliant with optimal brace wearing the success rate is in the order of 80 percent and so in these patients an operation is avoided.
There is no standard approach to bracing for AIS. However, there is widespread general agreement that in the skeletally immature patient bracing may be purposefully undertaken with some curves in the 30-40 degree range. It is also agreed that before bracing is instituted there must be an x-ray documented progression of at least five degrees. The reason for this restriction is that one-third of AIS curves more than 30 degrees do not progress if nothing is done. The reason for the stabilisation of such curves is unknown.
Every spinal surgeon has a somewhat different approach to bracing for scoliosis and this should be explained in depth to the patient and the parents when this option is being considered. More information on bracing in scoliosis
Surgery
The last twenty years have seen major advances in surgical techniques for the correction of spinal deformity from all causes. The basic principle is to apply some form of internal fixation to the spine and to correct the curve within the limits of safety. This may be carried out by one of many techniques but usually involves the application of stainless steel rods, hooks and screws to the spine in the corrected position and, most important, to join the vertebrae together by a spinal fusion with bone graft from the patient’s pelvis. The indications for a particular technique is influenced by many factors. The spinal surgeon uses the method that works the best for him/her and should be explained in detail to the patient.
Surgery for AIS has been made very safe by the use of spinal cord monitoring during the operation. Here the electrical activity in the spinal cord is monitored at crucial stages of the operation to ensure it is not at risk. Nowadays, AIS patients give their own blood prior to operation so that they can be transfused with this if necessary.
Surgery for AIS produces excellent results and where indicated can be recommended with confidence. In the long-term the only restrictions that are placed on the average patient is for participation in body contact/collision/high impact sports.
The post-operative routine varies from surgeon to surgeon and this too should be discussed in detail well before operation.
For those patients or parents who are interested in making an application to the Medical Services Advisory Committee to the Australian Government Department of Health concerning adding an item for Vertebral Body Tethering for Adolescent Idiopathic Scoliosis to the Medical Benefits Scheme, you may do so at the link below.
Vertebral Body Tethering is a growth modulation surgical therapy. It is usually used in AIS. View a Public Summary Document – Vertebral Body Tethering for Adolescent Idiopathic Scoliosis from the MSAC dated 25-26 November 2021.
Also, you may like to view an information webinar posted on YouTube in December 2023 by Setting Scoliosis Straight titled Vertebral Body Tethering vs Spinal Fusion. Topics include:
- Introduction
- Pros and Cons of VBT vs Fusion – Presented by Firoz Miyanji, MD
- Summary of the most impactful latest VBT research – Presented by Noelle Larson, MD
- Quantification of Motion in VBT vs Fusion – Presented by Peter Newton, MD
- Which patients are indicated for VBT and which are NOT and WHY? – Presented by Daniel Hoernschemeyer, MD
- Spinal Fusion Patient Story – Presented by Sammi S.
- VBT Patient Story – Presented by Makena W.
Spinal surgery MBS item changes to exclude use for Vertebral Body Tethering (VBT)
From 1 March 2024, spinal instrumentation items 51021 to 51026 and 51165 for anterior exposure of the spine will be amended to exclude their use for VBT for the treatment of scoliosis. View the Australian Government Department of Health’s Fact Sheet concerning this change.
